Since the passage of the US Affordable Care Act (ACA) in 2010, analysts have been making bold predictions about which segments of the health insurance market would grow—and which would contract. It has been widely reported that the individual segment and private exchanges were poised for strong growth, while the employer segment was viewed as a dying market.
But these predictions were wrong.
Individual segments have massively underperformed. The death of the employer segment has been greatly exaggerated. Only the government segment has met expectations, with an ongoing shift to Medicare Advantage and the ACA drawing millions of previously uninsured people into Medicaid.
Abrupt shifts in health plan profit pools have had real-world impact. In 2014, the industry reported exchange-related losses of nearly $3.5 billion—and major losses were reported in 2015 as well. Health Care Service Corporation, the Chicago-based parent company of several Blue Cross Blue Shield plans, announced losses of $1.5 billion in its individual business in 2015. UnitedHealthcare reported $75 million in ACA-related losses in 2015 and expects to lose more than $500 million in 2016. Insurance coops in many states, including Colorado, Kentucky, Nevada, and New York, have closed their doors, and this trend is expected to continue, as coops betting on risk corridors to keep them solvent now have no choice but to price at market levels.
It’s time to take a step back and assess where the big shifts are really occurring in the health insurance landscape and where dollars are flowing. Adjacent profit pools, such as specialty insurance, are becoming increasingly attractive as they expand in scale and offer a way for health plans to recapture margin lost during conversion to administrative services only (ASO) models. What’s more, downward revenue pressures coupled with high medical cost inflation are changing the relationship and value proposition of payers and providers, all but forcing payers to take a more active role in care delivery. With so much in flux, payers need a clear understanding of how the health care industry is changing—and what capabilities will be needed to win.
Big Shifts in Classic Profit Pools
Our analysis of the individual, employer, and government segments identified several key insights that have not been fully recognized in the marketplace. In our view, the individual segment is unattractive. Even with margin improvement, it will remain a small part of the market. Employer segments still represent the largest profit pool and will continue to grow over time. Meanwhile, the government segment represents a rapidly growing opportunity, albeit one in which it is increasingly tough to compete.
The individual segment will continue to underperform. The individual segment has grown from a small, niche product into a mainstream market. Even so, it has remained largely unprofitable and has significantly underperformed. It is likely to continue its pattern of slow growth for two reasons. First, small groups have not dumped their health plans at the high rates analysts expected, and therefore fewer employees have been compelled to seek individual plans. Second, the ACA’s reinsurance and risk corridor programs, designed to stabilize premiums and protect payers that take on sicker, costlier enrollees, were never fully funded and will end in 2016.
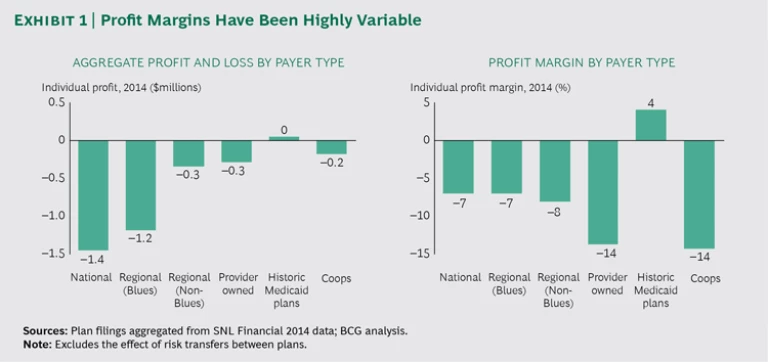
Payers that have been pricing below cost on the exchange, relying on government programs to cover their losses, will be forced to either increase prices on a highly price-sensitive customer base (especially for subsidized consumers) or exit the market. Plans that made significant bets on the exchange (and off exchange) will need to reexamine the merits of those choices. With widely varying profitability and no clear winning strategy, even profitable plans have taken on sizeable regulatory risk and considerable expense, in both their investment dollars and company resources. (See Exhibit 1.) Even if pricing and margins stabilize in the individual segment (and assuming there’s no large-scale employer dumping, which we don’t expect), total profit pools will reach just $2 billion, a small fraction of the profits generated by other segments.
Employer profit pools are still a cash cow. With an improving economy and steady employment rates stoking the competition for talent, the employer-sponsored insurance (ESI) segment is still strong. We expect the erosion of small-group segments to be minimal and overall profits in this segment to grow, not shrink. And while an increasing number of employers in large-group segments are moving to ASO, the majority of companies intending to transition to ASO have already done so. As long as payers can keep medical costs under control, the relative margin of this segment will outperform Medicare and Medicaid, and absolute profits will grow. In short, a substantial self-funded and fully insured ESI segment still represents an excellent bet for companies with the right capabilities.
Payers will be wise to invest in the capabilities increasingly demanded by employers. These include improved clinical analytics and reporting, enhanced medical management programs, and tightened integration with other clinical assets, like telemedicine and on-site clinics. It also means continued evolution of the distribution channel in response to employers’ increasing demand for sophisticated support both at the time of purchase and on an ongoing basis. Payers that underinvest in ESI business do so at their peril, leaving sizeable profits and expansion opportunities on the table.
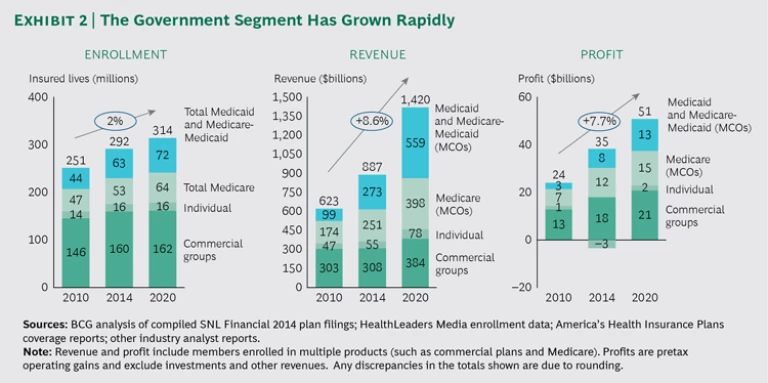
The government segment will grow, but margin compression is a threat. The government segment has grown rapidly, and is expected to continue growing at a compound annual rate of 5% through 2020; enrollment in Medicare and Medicaid is expected to increase steadily through 2020, generating billions in revenue and profit. (See Exhibit 2.) But the segment’s future is closely tied to the Centers for Medicare & Medicaid Services, a federal agency that is susceptible to enormous fluctuations in response to the political climate and changing regulations. The recent cuts in Medicare Advantage funding and increased oversight of rate setting for Medicaid are just two examples.
To thrive in the government segment, companies must cater to the needs of the highly complex Medicare and Medicaid populations, while keeping costs under control. Due to changes driven by the ACA, this segment has become increasingly sensitive to rising health care costs and will continue stepping up efforts to control spending. This will inevitably put additional pressure on margins. In response, payers will need to effectively manage care utilization and hang on to ESI business as an important source of profitability.
A Rise in Adjacent Opportunities
In addition to thinking carefully about where to invest (or divest) resources in the core insurance segments, payers need to consider how best to seize the advantage in emerging profit pools. There are large-scale changes happening outside of the core insurance business—in segments like specialty pharmacy, dental, vision, and behavioral health—and payers can position themselves to capitalize on these trends.
Pharmaceutical cost inflation drives up medical costs. Pharmaceutical costs are rising. As patents expire on blockbuster drugs, many pharmaceutical companies are turning to personalized medicine as the next frontier. Specialty drugs now account for one out of every three dollars spent on prescription drugs, and their costs are expected to grow another 19% in 2016. These drugs already represent 42% of the current drug pipeline and could account for 9% of all health expenditures by 2020.
The industry experienced a similar period of high medical inflation during the 1990s and in the first decade of this century. Two strategies—vertical integration and partnerships—helped companies mitigate the effects. But companies can also more aggressively capitalize on the opportunity. Given the present-day emphasis on pharmaceuticals and specialty drugs, payers may need to rethink their pharmaceutical management strategies by expanding capabilities along the value chain in areas like advanced utilization management (evaluating the necessity and appropriateness of using health care services) and step therapy management (providing patients with the most cost-effective drug therapy and progressing to more costly or risky therapies as necessary). For some payers, it may even be time to bring some components of pharmacy benefit management back in-house.
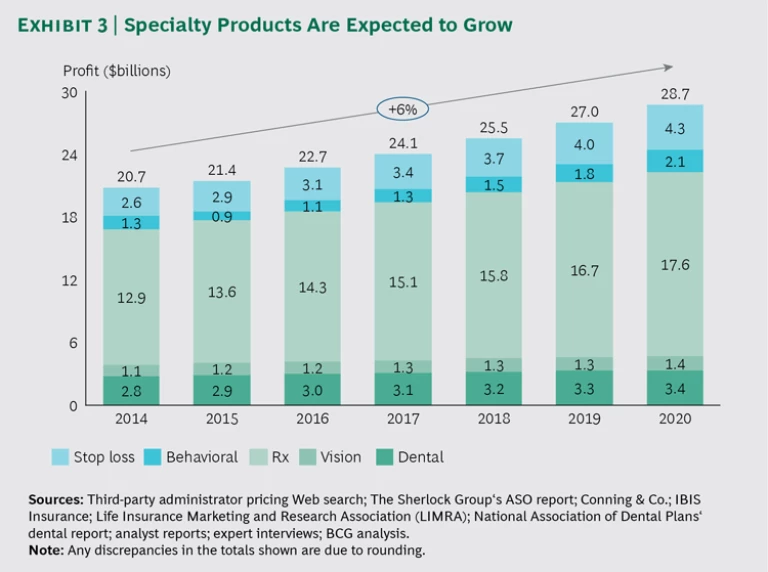
Specialty segments are becoming a core capability. Business segments that were formerly considered adjacent or add-ons are becoming a core profit pool. Specialty services, such as dental, vision, and behavioral health, will continue to grow. (See Exhibit 3.) This is yet another reason why the commercial segment remains highly attractive: there is a significant growth opportunity in these adjacent areas. To fully maximize the ESI group opportunity and seize share in the specialty segment, health plans need to rethink their core capabilities. As more employers move to self-insurance, a payer’s ability to supplement lower ASO profits with add-on products will dictate its success in ESI. Payers may need to revisit prior decisions to outsource specialty services to third parties and instead bring these capabilities back in-house.
The Imperative of Payer-Provider Collaboration
Historically, payers’ relationship with providers was based on a straightforward transaction: reimbursement for services delivered. But several trends in health care—including growing attention to value-based health care, patients’ increased cost sensitivity, and new medical loss ratio requirements (under which insurance carriers must submit data that shows the percentage of premium dollars spent on clinical services, as opposed to administrative costs and profit)—have prompted payers to more actively partner with providers in an effort to decrease health care utilization and improve population management.
There are signs that both sides are beginning to soften the decades-old stance that “my loss is your gain,” and some are beginning to embrace the notion that payers and providers, as well as patients, can mutually benefit from decreased costs and improved clinical outcomes. While there is a great deal of activity in the market, there is little consensus on how payers and providers can collaborate most effectively. A wide variety of models are being tested, from simple bonus payments that reward efficiency to tightly integrated partnerships—such as Aetna’s recent venture with Inova—in which payers and providers share costs and profits.
At the same time, providers have begun to launch their own health plans, increasing competition for risk premiums and insurance dollars. There are currently 150 provider-owned health plans in the US, with approximately 10 to 20 new entrants each year. Launching a health plan requires providers to take on more risk, but they also retain all the associated cost savings. In addition, existing plans are expanding their geographic reach through acquisitions. Kaiser’s purchase of Group Health Cooperative, for example, will add an eighth market to the consortium’s operations. Catholic Health Initiatives, which moved into insurance in 2012, is already operating in 19 states.
These trends leave payers with little choice but to increase their participation in care delivery if they want to capture a meaningful share of ESI and government profit pools. While increased participation could come in the form of stronger provider relationships or even direct entry into care delivery (as UnitedHealthcare’s Optum subsidiary has done with Monarch’s management company), the profit pools being created will make it increasingly hard for traditional standalone players to compete without some level of clinical integration.
Shifting trends in the health care industry have huge implications for payers. Profit pools are moving away from payers’ core competencies and funneling into adjacent services. Companies that choose to double down on the same old business model will gradually lose market share as these trends take hold. But companies with a clear-eyed understanding of where the market is heading can build up their capabilities and skill sets to take a leadership position in these profitable sectors. By capitalizing on industry changes, payers have an opportunity not only to protect their current market position but also to uncover new sources of sustainable profit for decades to come.