Introduction
Santeon, a Dutch network of seven leading teaching hospitals, has achieved reductions of nearly 30% in unnecessary inpatient stays and up to 74% in the rate of reoperation due to complications in breast cancer patients. Santeon achieved these results in a year and a half, not merely by meeting protocols or guidelines—its member hospitals have been doing that for a long time—but by emphasizing transparency and making value delivered to patients the core of its strategy.
The key to Santeon’s success was the implementation of a structured, value-based health care (VBHC) approach. In 2015, BCG started working with Santeon to make VBHC a reality at its hospitals. After an initial design phase, Santeon began implementing VBHC in March 2016 among five patient groups: breast cancer, prostate cancer, lung cancer, cerebrovascular accident (CVA), and hip arthrosis. Implementation in each group consists of four stages:
- Use a multidisciplinary team to define the right metrics to improve outcomes.
- Share and learn internally, and then initiate a strict and simultaneous cadence of improvement cycles within the member hospitals.
- After a few internal cycles to validate and stabilize the process and data, share results externally to accelerate improvements.
- Engage with patients and payers to move toward value-based contracting.
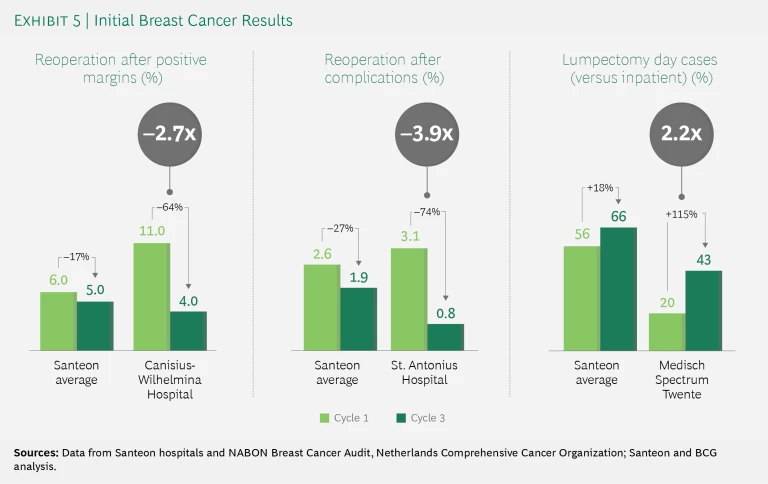
The breast cancer group was the first to reach the third stage. After defining a short list of key metrics for outcomes, costs, and process indicators (stage 1), Santeon began sharing data within and among its seven hospitals to foster internal learning in a safe environment (stage 2). Now, following the completion of three improvement cycles, the results are being shared with the outside world on a hospital-by-hospital basis (stage 3). Those results are very impressive indeed. In addition to the figures noted above, Santeon achieved, on average, a reduction of more than 15% in lumpectomy reoperation rates after positive margins, with one hospital achieving a reduction of about 60% (from 11% to 4%).
Other Santeon patient groups show similar signs of improvement, although they are not yet at a sufficiently advanced stage for the results to be published externally. Still, the variation observed in the metrics data among the hospitals for the other patient groups is comparable to that seen in the breast cancer group and clearly indicates the potential for improvement (for 30% of the metrics, Santeon found that the highest and lowest scores varied by a factor of between two and five, indicating significant improvement potential in those domains).
In this report, we share Santeon’s successes in implementing VBHC, describe how the hospital group has made the transformation work, and offer a number of key lessons for other providers whose ambition is to put value for patients at the center of their approach to health care.
THE SANTEON VBHC MODEL
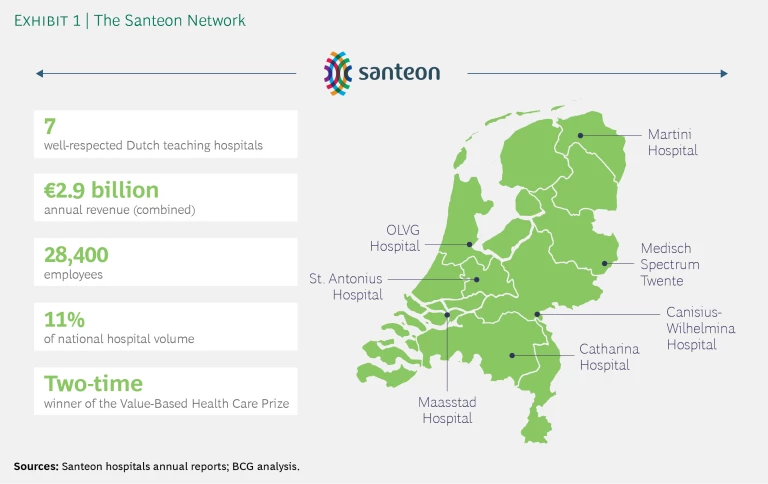
Santeon is a cooperative of seven top-performing Dutch hospitals that together account for 11% of the nation’s hospital care volume, employ approximately 29,000 people, and generate €2.9 billion in annual revenues. Santeon represents a unique effort by hospitals that have joined forces to increase the quality and efficiency of patient care. The hospitals are widely dispersed across the Netherlands and do not directly compete with one another. (See Exhibit 1.)
Santeon embraced the VBHC concept in 2012 and between 2015 and 2017 worked with BCG on various projects to put VBHC at the core of its collaboration model. Santeon is now widely recognized in the Netherlands and beyond as a VBHC pioneer and a driving force and partner in the movement toward a more value-based health care system. (See “The Promise of Value-Based Health Care.”)
THE PROMISE OF VALUE-BASED HEALTH CARE
THE PROMISE OF VALUE-BASED HEALTH CARE
Value-based health care aims for the best patient outcomes for every euro spent. Many articles have described the concept since Michael E. Porter and Elizabeth Olmsted Teisberg introduced it in Redefining Health Care: Creating Value-Based Competition on Results (2006). VBHC makes the delivery of improved health outcomes for the same or lower cost the primary objective of global health systems. The potential for improvement in health care value is enormous, given the large variations that exist among providers in treatment decisions, cost of care, and patient outcomes. The exhibit below shows the differences in outcomes among hospitals at the national level. Similar variations among hospitals are found across treatment areas and geographies.
In many industries, a difference in costs or quality of 5% to 10% between competing organizations typically triggers major improvement programs by the trailing organization. Among hospitals worldwide, the differences in cost and quality can range from 400% to 3600%! The failure to act on such large disparities reflects what Porter calls the “pre-industrial nature of health care.”
The VBHC approach emphasizes the systematic measurement of health outcomes and of the costs involved in delivering them to specific subpopulations—for example, to all patients who suffer from a particular disease or condition, such as colon cancer, or who share a similar risk profile, such as the multimorbid elderly. Teams composed of clinical specialists use this data on outcomes and costs to devise customized interventions that, over time, will improve the ratio of positive outcomes to costs for each patient group.
Focusing on the objective of improving health care value, VBHC has the potential to deliver better health outcomes at lower costs than are currently achievable by most health care systems around the world. VBHC also improves patients’ access to suitable care, identifies significant innovations in treatment and care delivery, and offers major new public- and private-sector business opportunities for health care organizations. VBHC promises to be a solution for hospitals that aim to deliver the best possible care for their patients while facing ever-increasing pressure from rising costs and a high registration burden around process metrics, guideline adherence, and reimbursement administration.
More and more health care organizations recognize the potential of VBHC and are moving toward a value-based way of working. Implementing VBHC is not merely a project; it transforms hospitals into learning organizations that provide care around patient groups, based on transparency in their outcomes and costs per medical condition.
Three Foundations of Success
Santeon’s success is based on three imperatives that it established before it began implementing VBHC around patient groups:
- A Shared Ambition and Long-Term Commitment to VBHC. The boards and medical leadership of each of the seven Santeon hospitals share an ambition to “realize better outcomes for patients faster together” via transparency on health outcomes and costs. They also committed to a long-term VBHC agenda: start with a few patient groups to develop and test a methodology and then expand it to include 20 to 25 patient groups by 2020.
- Establishment of a VBHC Model. Santeon designed and implemented the same VBHC model in all seven of its hospitals so that it could benchmark and leverage the network’s combined expertise efficiently. Multidisciplinary clinical teams organized around patient groups develop an aligned view across the seven hospitals on the 15 to 20 metrics that define value for each group. They then set up improvement cycles of six months each that establish a strict, simultaneous cadence for the teams in each hospital to follow. Hospitals develop and execute improvement initiatives locally, with input on data and best practices shared among them.
- The Right Infrastructure and Governance. Santeon established a central infrastructure and governance system to promote the VBHC model. First, it installed a central team comprising a VBHC program manager and a few data analysts to support the local multidisciplinary teams. This team ensures alignment across the seven hospitals, provides quality control, and helps local teams prepare and manage meetings. Second, VBHC became a key element in the governance of both the Santeon group and each individual hospital. For example, VBHC is now a standard topic on the agenda at board meetings, and the boards are responsible for making overarching decisions regarding investment, prioritization of the rollout of patient groups, and other matters. Third, a handbook was developed to codify the VBHC model, ensure uniformity, and provide guidance to stakeholders. The handbook describes the process and goal of each step within every improvement cycle, the roles and responsibilities of the participants in each cycle, the formats to use, and strict rules about data quality and the sharing of data internally and externally.
Implementing VBHC in Patient Groups
Prepared with a shared ambition, a working model, and the necessary infrastructure, Santeon began rolling out VBHC for the first patient groups early in 2016. The VBHC team for each patient group has a clear path to follow, consisting of four stages:
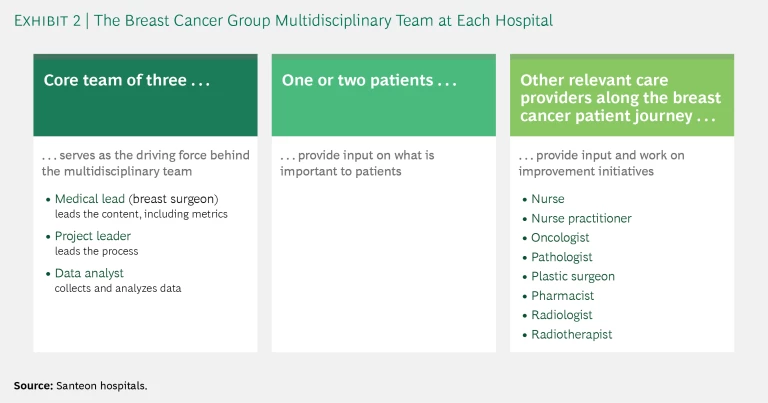
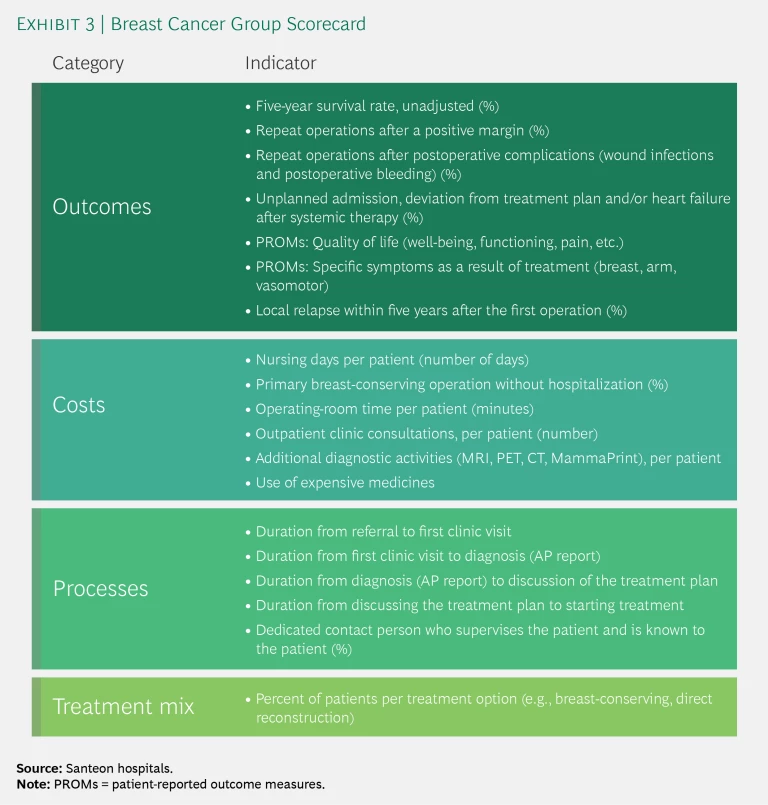
- Organize multidisciplinary teams and define the metrics. VBHC implementation within a patient group starts with forming a multidisciplinary team at each member hospital. Three core members are the driving force of each team and coordinate discussions among the seven hospitals. (See Exhibit 2.) Supported by a few central resources, one hospital takes the lead in developing a scorecard identifying 15 to 20 key outcome, cost, and process metrics relevant to its patient group. (See Exhibit 3.) It’s important for hospitals to be pragmatic about these scorecards, leveraging existing registries as much as possible and starting with metrics for which data are readily available (refining them over time if necessary). For outcome metrics, Santeon uses the International Consortium for Health Outcomes Measurement (ICHOM) indicator sets as much as possible. (See the sidebar “ICHOM’s Global Standards for Health Outcomes Measurement.”) For cost metrics, it identifies the biggest cost buckets for a patient group and the most important cost drivers to track. Santeon adds process metrics only when they are critical for patients (such as the duration of the period of high uncertainty between diagnosis and the determination of a treatment plan). Patients play a central role in defining all metrics related to the outcomes and processes that matter most to them.
ICHOM’s Global Standards for Health Outcomes Measurement
ICHOM’s Global Standards for Health Outcomes Measurement
The International Consortium for Health Outcomes Measurement (ICHOM) is a nonprofit organization cofounded in 2012 by Michael Porter of the Harvard Business School, Martin Ingvar of the Karolinska Institute, and The Boston Consulting Group. The consortium’s mission is to transform health care systems worldwide by measuring and reporting patient outcomes in a standardized way.
ICHOM convenes global teams of physician leaders, outcomes researchers, and patient advocates to publish standard sets, which define the outcome measures that matter most to patients. The organization also supports health care providers worldwide in implementing and measuring these outcomes in practice, which ultimately places patients at the center of health care delivery, and in the process drives up the quality of care and reduces costs.
As of May 2018, ICHOM had collaborated with 658 working group members representing 44 countries and had published 23 standard sets (9 more are in the pipeline). The exhibit below illustrates ICHOM’s standard set for breast cancer.
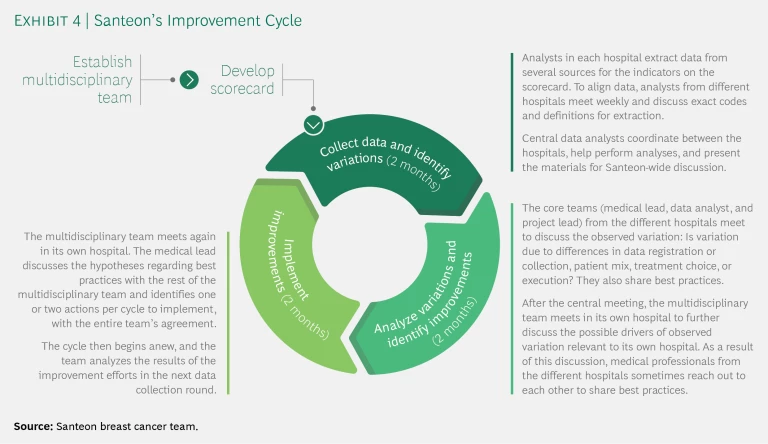
- Share results internally and implement a standardized improvement cycle for each patient group. When teams and scorecards are in place, teams embark on the improvement cycle: a continuous feedback loop that involves collecting data, analyzing data, identifying areas for improvement, and implementing improvement initiatives. (See Exhibit 4.) A safe learning environment is critical at this stage. Therefore, data and results from the first three six-month improvement cycles should be transparent only among member hospitals and not yet shared with external parties. Teams use this data not to judge one another but to form hypotheses regarding potential improvement initiatives and develop best-practice sharing on the basis of observed, clinically relevant differences. These differences are not necessarily statistically significant; making that a prerequisite to taking action could create unwarranted delays. As soon as a team seems to be performing better, it makes sense to look at it more closely and share approaches. Confidential sharing lets the teams gain familiarity with the new way of working and approaching data, highlights areas where improvement is possible, and allows time to make the first round of improvements and validate the comparability of data before going public.
- Share results externally to inspire others and accelerate the improvements. The teams know that the aim is to share the data externally after three improvement cycles. This can encourage other hospitals to measure and share the same metrics, providing the health care community with an even broader pool of data to learn from. In addition, sharing results externally can accelerate improvement initiatives. Santeon collects its data in an outcome database, which provides researchers with a rich pool of data that they can use for future research, with the aim of publishing scientifically and statistically significant results over time.
- Move toward value-based contracting. Leveraging transparency around health outcomes, the appropriateness of care, and the long-term effects of treatment for contracting with health insurers or public payers is the logical next step. Today, many hospitals still receive reimbursement for care on the basis of volume rather than value. This makes it harder for providers to reap any direct financial benefit when they improve the quality of the health care that they deliver. Santeon is working with health insurers in the Netherlands to move toward value-based contracting, and it recently became the first health care organization in the country to announce such contracts for breast cancer, with three insurers.
2 2 Santeon partnered with the Dutch private health insurer Menzis to cofinance the first period of implementing value-based improvement cycles in its hospitals.
THE IMPACT OF SANTEON’S MODEL
Evidence that Santeon’s VBHC approach is working is emerging from the breast cancer group, which has already reached the external transparency stage, as well as from the other four patient groups (hip arthrosis, lung cancer, prostate cancer, and CVA), which have not yet reached that stage.
The Breast Cancer Group
Santeon’s multidisciplinary breast cancer teams, the first to complete three improvement cycles, recently revealed their first results externally.
- Reoperations due to positive surgical margins fell by 17% across Santeon and at Canisius-Wilhelmina Hospital (CWZ) declined by more than 60% (from 11% to 4%). In the first improvement cycle, Santeon observed a factor-4 variation between the lowest and highest percentages of reoperations due to positive surgical margins (which indicate that some cancer cells may remain) after lumpectomy. CWZ, which had the highest percentage of such reoperations, analyzed possible causes and implemented three corrective measures: using echography during surgery to gain more certainty about having removed all cancer cells, improving communication between surgeons and pathologists on the definition and risks of a positive margin, and more explicitly discussing whether reoperation is the most sensible response to instances of positive margins. Data collection one year later (in the third improvement cycle) showed an impressive reduction in reoperation rates due to positive margins at CWZ. The team will continue to closely monitor this indicator in future improvement cycles to ensure a lasting impact.
- Reoperations due to postoperative complications after lumpectomy dropped by 27% across Santeon and at St. Antonius Hospital declined by more than 70%. Although complication and reoperation rates were low in all member hospitals, a factor-4 variation between the lowest and highest percentages of reoperations after postoperative complications led the teams to investigate improvement opportunities. The safe, confidential setting established by Santeon’s VBHC model enabled the St. Antonius Hospital breast cancer team to compare the outcome scores of individual surgeons. The team found that one outstanding performer used much more intensive wound flushing during surgery. St. Antonius surgeons who then adopted this practice saw an immediate reduction in complication rates, and data from the third improvement cycle confirmed the improvement, showing a 74% decline in reoperation rates after complications.
- Santeon reduced the number of days in the hospital for lumpectomy patients by increasing the number of day cases by 18% on average, and Medisch Spectrum Twente doubled its day case (versus inpatient stay) rate. Data collected in the first cycle indicated that day case treatment percentages for lumpectomy, which the teams expected to be around 85%, in fact ranged from 20% to 79%. After testing several hypotheses, including correlations with age and home situation, the teams found that two factors had a direct effect on whether patients could go home on the day of surgery. First, some patients were not aware in advance of the expected discharge date; when it was made clear that they could go home on the day of surgery if there were no complications, patients were able to adjust their arrangements accordingly. Second, at hospitals that employed full anesthesia followed by morphine, patients were often unable to go home on the day of surgery. But at hospitals that relied on locoregional (nerve block) anesthesia, patients could go home with over-the-counter pain relievers on the same day, with no additional negative effects. Changes that give preference to locoregional anesthesia when appropriate increased the number of day cases within six months.
The Hip Arthrosis, Lung Cancer, Prostate Cancer, and CVA Groups
The VBHC teams in Santeon’s other four initial patient groups are now either finalizing the second improvement cycle or have started the third. (Santeon also recently started the first improvement cycle for patient groups focused on kidney disease, colorectal cancer, and childbirth.) Consistent with VBHC principles to protect a safe and open learning environment, data sharing at these early stages is restricted to internal teams and cannot yet be disclosed in this report. Nevertheless, some anonymized examples offer a preliminary view of select initiatives launched to improve outcomes, costs, and processes.
Member hospitals are making changes to improve outcomes for patients.
- To improve postoperative outcomes in lung cancer patients, one hospital changed its approach to biopsies. The lung cancer team found that postoperative complication rates, lengths of stay, and surgery durations all varied by nearly a factor of two. At one hospital with unfavorably high rates on all these metrics, the team undertook a local improvement initiative. It found that, as standard practice, other Santeon hospitals took diagnostic biopsies preoperatively (instead of performing intraoperative frozen sections), and patients in these hospitals reported reduced uncertainty going into surgery. As a result, the advantages of preoperative diagnostic biopsies versus frozen section, which had previously been debatable, were now deemed sufficient to justify changing protocols. Over the next cycles, the lung cancer team will closely monitor the impact of the new approach.
- To reduce complications and postoperative lengths of stay in lung cancer patients, hospitals are testing new drain protocols and equipment. The longer a patient has a drain, the higher the risk of infection, which can extend the length of stay at the hospital. Member hospitals observed variations in complication rates and lengths of stay, and subsequently found a factor-2 variation in the timing of drain removal, as well as differences in drain protocols. The lung cancer team discovered that the best-performing hospital, rather than letting doctors continue a drain when they were unsure if it had done its work, used pressure-testing equipment and prescribed the pressure at which a drain can be removed. A Santeon-wide protocol is now under development.
Member hospitals are reducing costs by eliminating practices that do not contribute to better outcomes:
- Hospitals are adopting best practices in patient flow management for hip arthrosis patients to reduce unnecessary preoperative days in the hospital. The hip arthrosis team’s first improvement cycle revealed differences in the number of preoperative days among the Santeon hospitals. Most Santeon hospitals admit the majority of their hip surgery patients on the day of surgery. Some, however, admit patients a day in advance for blood tests. Orthopedic surgeons discussed this disparity—and a solution that other hospitals use to overcome it—at a semi-annual VBHC meeting. The solution is now being implemented at one hospital.
- Fewer postoperative X-rays are being taken in hip arthrosis patients, following a finding that some photos did not contribute to better health outcomes. Variation by a factor of three in the number of X-ray photos taken per patient motivated the teams to compare the extent of diagnostic imaging throughout the patient journey at different member hospitals. The hospital where the largest number of photos were taken was unique in taking them in the recovery room immediately after surgery, despite the absence of any observable differences in health outcomes. On the basis of this finding, the hospital stopped taking these unnecessary X-rays, which lowered costs without jeopardizing outcomes.
Member hospitals are changing processes to improve the patient experience:
- For prostate cancer patients, the new standard calls for inviting a family member or caregiver to appointments where diagnostic results are discussed. This measure was implemented following a suggestion by a patient—a member of the VBHC team—who had received an unexpected terminal diagnosis without a family member or partner present. He considered this the most undesirable way to receive such impactful news. The hospital subsequently changed its policy and invites family members and caregivers to all diagnostic result appointments, whether the results are positive or negative.
- For CVA patients, one hospital is working to improve patient communication regarding the expected length of stay by increasing the frequency of discharge discussions in the wards. Patients on the VBHC team asked for better and timelier communication about the inpatient stay. Comparing data and patient experiences across Santeon hospitals, the VBHC teams found that hospitals that held more frequent discharge discussions tended to provide more accurate and up-to-date briefings to their patients, whose hospital stays were shorter. One hospital is therefore preparing to switch from twice-weekly to daily meetings.
In light of the proven benefits for both patients and clinicians, Santeon plans to roll out value-based health care to 20 to 25 additional patient groups by 2020.
SEVEN KEY LESSONS FOR OTHER HOSPITALS
Santeon’s experiences with VBHC already offer a number of valuable lessons for any hospital that is trying to improve health care quality while maintaining or lowering overall costs:
- Develop a common understanding of value and ensure long-term commitment. Medical specialists, patients, and external stakeholders unite around a shared ambition to create transparency and improve health care outcomes at similar or lower costs. An outspoken long-term commitment and a willingness to “make it real” are essential to achieving lasting change.
- Start small, be pragmatic, and create a snowball effect. Aim for a smooth start with a scorecard based on existing quality standards for a limited number of promising conditions. Prioritize based on clear criteria. For example, begin with conditions that have clear improvement potential and a fair amount of good data available, with doctors who are enthusiastic or who are already implementing VBHC in isolation. Give the VBHC champions a platform. This will generate enthusiasm for the VBHC approach and lay the groundwork for expansion into more complex areas.
- Build a safe learning environment, and keep up the pace toward transparency. A period of internal data sharing only helps VBHC participants gain confidence in comparing outcomes and testing improvements. Maintain the focus and momentum by emphasizing the prospect of external communication and, ultimately, active cooperation around value with external stakeholders, including insurers.
- Have medical professionals take the lead, and provide them with process support. To build on their expertise and intrinsic motivation, let medical specialists lead team discussions and select the relevant metrics. Nonmedical tasks require an investment in extra resources to manage the project, facilitate processes, drive improvement initiatives, and provide data and analyses.
- It’s about the patient—and must be implemented with the patient. VBHC puts patient value at the core of decision making. To emphasize this perspective and foster the right mindset among all participating professionals, every Santeon VBHC team has one or two patient members. Santeon has gained valuable insights from their points of view, and patients indicate that they appreciate seeing the results of their participation. (See “Patients See the Direct Impact of Their Contributions.”)
Patients See the Direct Impact of Their Contributions
Patients See the Direct Impact of Their Contributions
VBHC teams engage directly with patients in order to understand the outcomes that matter most to them. In many cases, patients’ suggestions for improvement can be adopted quickly.
“Awaiting the results of mammography, at home, is a most horrible period filled with insecurity. Sharing this in the VBHC team led to tangible impact: mammography results are now communicated on the same day.” — patient of breast cancer VBHC team
“All patients are now actively encouraged to bring a second person to consultations at the prostate outpatient clinic. This change was implemented based on my recommendation.” — patient of prostate cancer VBHC team
“Breast cancer patients now find soft facial tissues to dry their tears in the waiting room of the breast cancer outpatient clinic. This is the first impact I saw after sharing my experiences with the value-based health care team.” — patient of breast cancer VBHC team
- Improve locally, and learn from others. The local VBHC teams in each hospital are responsible for prioritizing and executing improvement initiatives. They use data from other hospitals as points of reference and comparison. Santeon hospitals benefit from coordinated data collection across seven hospitals, but hospitals that are not (yet) collaborating in a network can use publicly available data and international benchmarks, or start their own data-sharing alliances. The only prerequisite is that definitions be aligned. For this, ICHOM can provide a very useful starting point, as it has defined global standards for many disease areas.
- It’s hard work and moves one step at a time, but it’s absolutely worth it. Implementing VBHC is not a quick-fix solution, but it leads to groundbreaking and continuous improvements. It requires a real change effort from all involved—an effort that is well worth the investment, according to Santeon’s medical professionals. (See “Health Care Professionals Embrace This Way of Working.”) The VBHC approach appeals to the intrinsic motivation of medical professionals, because it focuses on what matters most to patients, and the impact of efforts to improve is clearly apparent.
Health Care Professionals EMBRACE This Way of Working
Health Care Professionals EMBRACE This Way of Working
VBHC allows doctors to share best practices and learn from one another in a safe and supportive environment. The focus is always on delivering better quality for patients while maintaining or lowering overall costs.
“This is an unbelievably good concept. Although it takes time, it is much more motivating than the other ways we have to look at data and deal with quality indicators. By learning from each other, we can really improve care for our patients. That gives me a lot of energy and I definitely recommend working like this to my colleagues.” — Yvonne van Riet, breast surgeon, Catharina Hospital
“For me, the power of collaboration is in directly getting feedback if something’s working or not. More contact about the content. A practical way to mold our profession together. Looking at the numbers more often and making plans for a new process. And adjusting the process faster.” — Ron Koelemij, oncological surgeon, St. Antonius Hospital
“This way of working stimulates us to improve ourselves. We discuss recognizable practical situations, and you have a conversation partner you know well. It helps; it makes it easier to talk to each other. You have the feeling of forming some kind of a club that is less anonymous, which makes talking easier.” — Luc Strobbe, surgeon, Canisius-Wilhelmina Hospital
Value-based health care is poised to transform the health care industry, improve patient outcomes, lower health care costs, and dramatically improve the patient experience. By creating transparency around differing approaches to care, comparing outcomes, and changing protocols accordingly, providers are gaining new insights into the ways specific treatments improve the health of patients. As the data on outcomes continues to grow and national registries become richer and more robust, the VBHC model will only become more compelling.